CME INDIA Case Presentation by Dr. N. K. Singh,MD, FICP, FACP,F RSSDI, F Diabetes India, Director – Diabetes and Heart Research Centre, Dhanbad, Dr. Prabhat Agrawal, Professor, PG department of medicine, SN medical college, Agra (Uttar Pradesh).
CME INDIA Case Study
How Presented?
- In August 2024, 54 yrs. old female with history of diabetes of six years duration consulted for blood sugar control. She had no specific complains. She was on metformin500 mg BD and telmisartan 40 mg OD.
- The physical examination was normal. BP-130/80 mmHg,BMI-23.4, Hb1Ac – 7.9 mg, Lipids-Normal, RFT/LFT-Normal.
- Her medication was modified as Vildagliptin 50 mg and Metformin 500 mg combination in BD dose.
- After 3-week, patient came with Gum swelling.
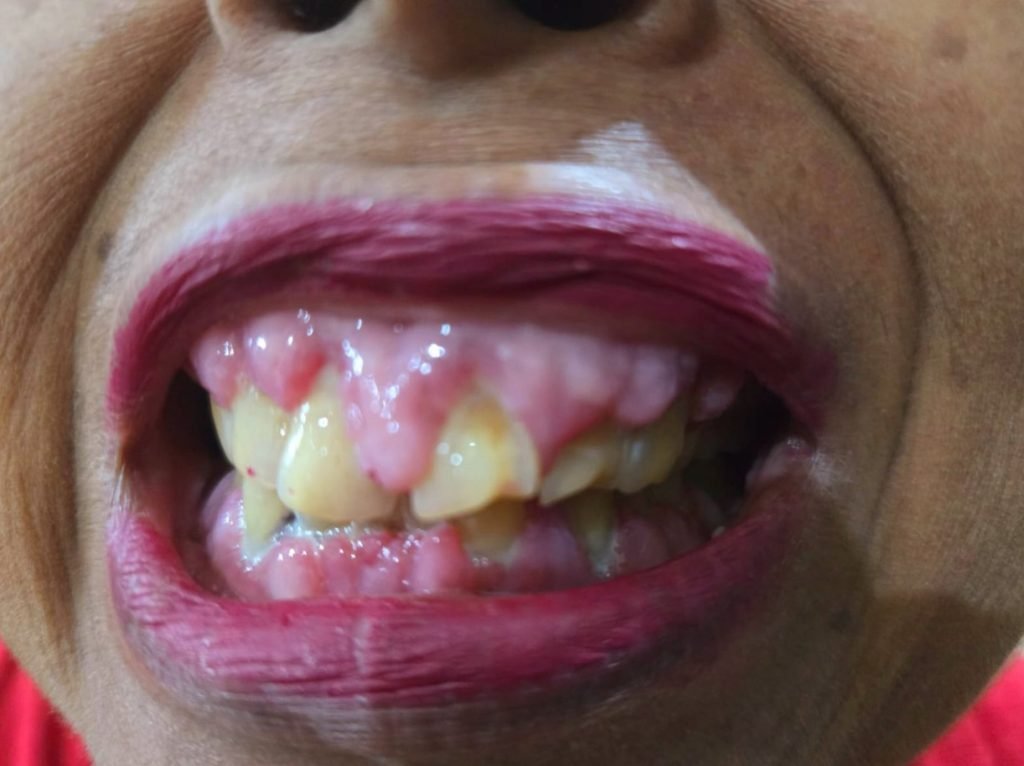
(13th August 2024 )
- It was Firm, painless, nodular enlargement of the interdental papilla, limited to the keratinized portions of the gingiva and extending to the facial and lingual gingival margins.
- It appears firm and pale pink with minute lobulations, pouting from underneath the gingival margin. This is delineated by a groove of tissue that does not bleed on touch.
What was done further?
- A periodontal examination did not show the presence of periodontal disease.
- Full mouth periapical radiographs and orthopantomography ruled out periodontal disease.
- A complete blood was normal.
- No tissue biopsy planned.
- Investigated, CBC,RFT,LFT,VIT C – All normal. Considering
- Vitamin C test- 1.2 mg/dL (0.4-2.0 mg/dL).
- Vildagliptin, it was stopped and Dapagliflozin, metformin combination started.
What is your opinion? Was it Vildagliptin Induced?
When patient visited for opinion and all tests came to normal, considering the possibility of Vildagliptin induced Gingival Hypertrophy, it was stopped and patient instructed to keep watch on swelling. As patient noticed that after one month swelling got remarkedly reduced, she continued the Dapagliflozin and Metformin combination. Her Blood sugar remained in normal range throughout.
Recently visited on 04/02/2025
O/E
Hb1Ac-6.9%
CBC/RFT/LFT-Normal
Oral Examination
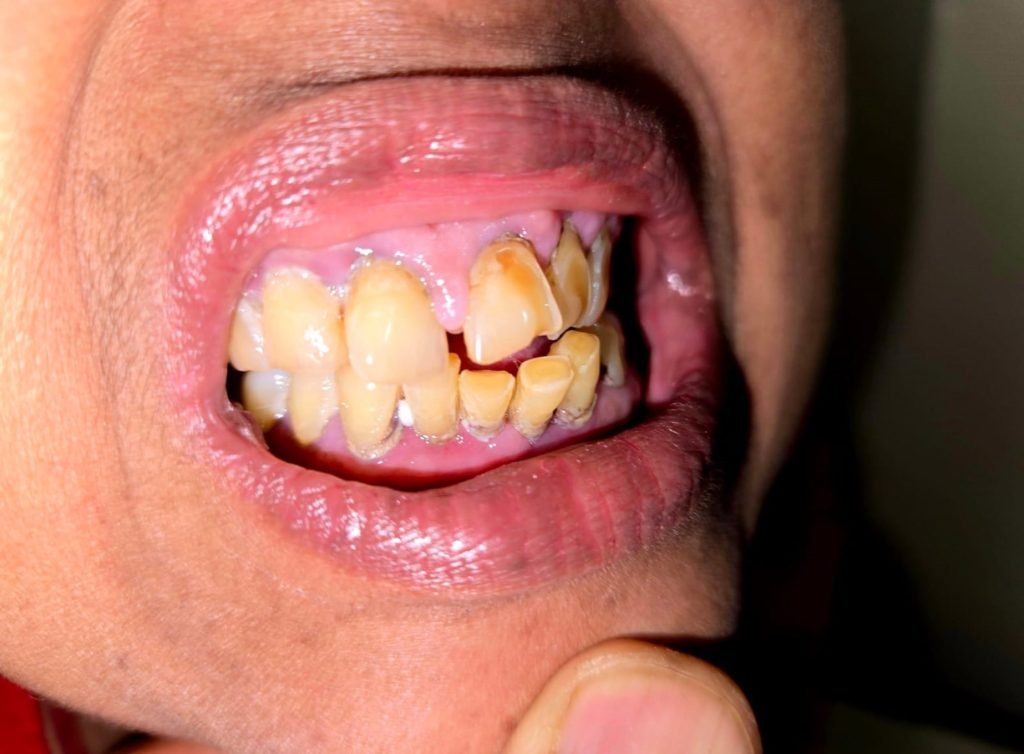
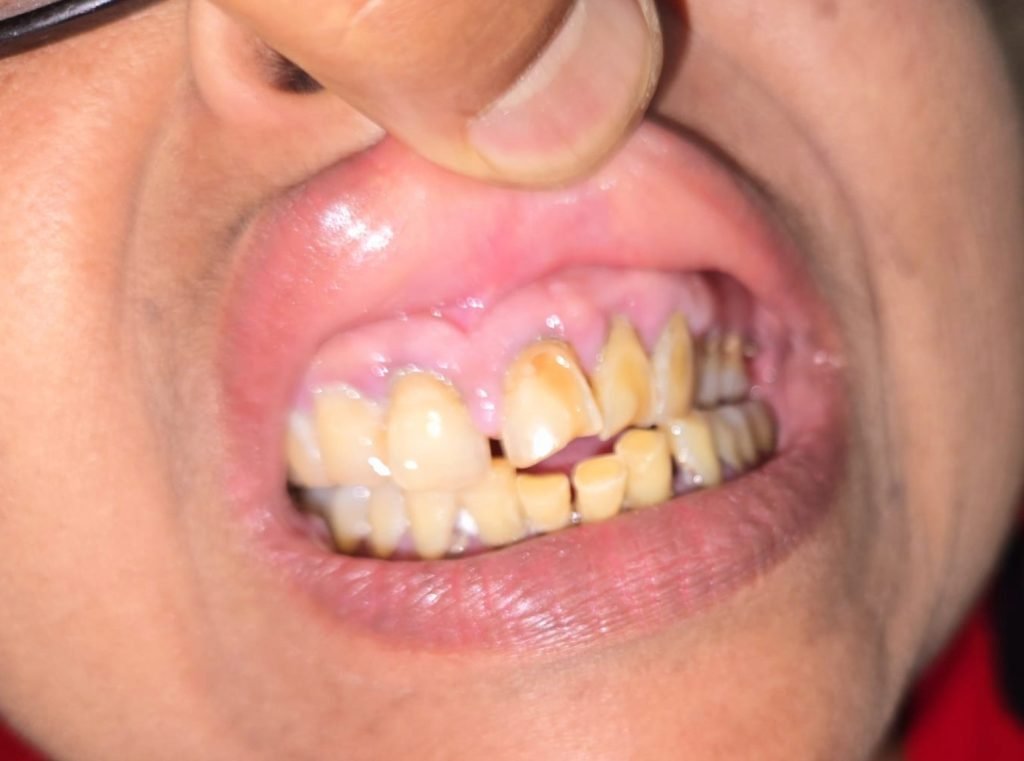
Diagnosis
- The diagnosis of drug-induced gingival overgrowth.
- Drug Implicated-Vildagliptin.
Differential Diagnosis
The differential diagnoses for DIGO (Drug-Induced Gingival Overgrowth) include:
| False Enlargement of Gingival Tissue: This condition appears as pseudo-enlargement due to an increase in the size of the underlying bone rather than the gingival tissue itself. Here, the gingiva remains normal. |
| Inflammation: Chronic inflammation manifests as red or purplish, smooth gingival tissue that is prone to bleeding upon contact. |
| Familial or Hereditary Conditions: |
| Familial Fibromatosis |
| Idiopathic Fibromatosis |
| Gingivomatosis |
| Hereditary Gingival Hyperplasia |
| These conditions lead to gingival tissue that is pink, non-tender, and has a firm, leathery texture. The enlargement typically affects the attached gingiva, the gingival margin, and the interdental papillae. |
| Physiological States: |
| Puberty: Hormonal changes can lead to gingival enlargement. |
| Pregnancy: Similar hormonal influences can cause gingival overgrowth. |
| Scurvy: A deficiency in Vitamin C results in gingival tissue that is extremely tender and prone to bleeding. |
| Systemic diseases: leukemia, tuberculosis, sarcoidosis, as their diagnosis can be corroborated hematologically |
Drug-Induced Gingival Overgrowth (DIGO)
DIGO is a side effect seen in patients taking anticonvulsants, immunosuppressants, or calcium channel blockers, influenced by genetic predisposition and plaque-induced inflammation.
| Anticonvulsants |
| Phenytoin (PHT) is the most common anticonvulsant linked to gingival enlargement, though sodium valproate, phenobarbitone, vigabatrin, primidone, mephenytoin, and ethosuximide can also contribute. |
| PHT and related drugs metabolize into 4-HPPH, which triggers gingival overgrowth. Multiple anticonvulsants used together can worsen the condition. |
| Immunosuppressants |
| Drugs like cyclosporin, tacrolimus, and sirolimus, used after organ transplants and in autoimmune diseases, are associated with gingival overgrowth. |
| Cyclosporin carries the highest risk, affecting up to 53% of renal transplant patients. Tacrolimus is less toxic and causes milder overgrowth, while sirolimus also shows potential for gingival enlargement. |
| Calcium Channel Blockers |
| Channel blockers like nifedipine, amlodipine, felodipine, and diltiazem can induce gingival overgrowth. |
| Amlodipine-associated cases have been reported within two months of initiation. |
| Patients on cyclosporin and calcium channel blockers, particularly nifedipine or diltiazem, have a higher risk of severe gingival hypertrophy due to drug synergy. |
What about DPP4-Inhibitors?
- So far, literature search to authors did not match any such corelation of DPP4 Inhibitors and Gingival hypertrophy. With present causal association and improvement this case becomes very illuminating due to its rarity.
- Eiji Nemoto et al observed that CD26 (DPP-4) expression was significantly induced on gingival fibroblasts when exposed to stimuli. This induction was evident both at the protein level and at the mRNA level). Given that periodontal disease involves local infections with specific bacteria, human gingival fibroblasts (HGF) are naturally exposed to a mix of inflammatory cytokines and various bacterial components, which likely contributes to this observed increase in CD26 expression.(Ref-6)
- Ironically, DPP-4 inhibitors, used in the treatment of type 2 diabetes, work by prolonging the activity of incretins. Notably, after periodontal treatment, there’s an observed increase in glucagon-like peptide-1 (GLP-1) levels, offering real-world evidence of a beneficial link between oral health and the incretin system. GLP-1 receptor agonists like exendin-4 have shown to promote osteoblast proliferation and development while counteracting glucose’s adverse effects on these cells. Furthermore, liraglutide, another GLP-1 receptor agonist, not only manages blood sugar but also exhibits anti-inflammatory and bone-protective effects. These outcomes advocate for the use of GLP-1 in both managing and preventing periodontitis in diabetic patients.(Ref-7)
- Although, we did not re-challenge this case with offending drug, DPP 4 Inhibitors.
CME INDIA Inputs
Dr. V. G. Nadgouda: Though rare, there are some reports of DPP-4 inhibitors (like vildagliptin) causing angioedema, oral ulcers, or mucosal inflammation. Since other systemic causes (infection, vitamin C deficiency, blood disorders, renal/liver dysfunction) were ruled out, stopping vildagliptin was a reasonable decision.
Dr. Suresh Chhatwani, Ahmedabad: CCB & Phenytoin cause gum Hypertrophy, but not heard about Vildagliptin. Some other cause/ poor oral hygiene with DM? Can be cause?
Dr. Prakash Wali, Kolhapur: If the gum swelling resolves after stopping vildagliptin, it strengthens the likelihood of a drug reaction. Periodontal infections, vitamin C deficiency, uncontrolled diabetes, or medication-induced gingival overgrowth (e.g., calcium channel blockers) have been already excluded in this case.
Dr. A.K.Virmani, Jamshedpur: Vildagliptin is notorious for any skin or mucous membrane reaction .Stopping it has led to improvements in this patient.
Dr. A. S. Deora: Luckily have never come across any side effect due to DPP4 i till date since their introduction in 2007-2008.Worth keeping in mind the possible side effect of DPP4i.
Dr. Meenakshi Sahapathi, Faridabad: DIGO patients present so fast after 3 weeks of medicine or after long duration of taking medication.
Dr. Rajiv, Bhagalpur: Generally speaking, an exposure of 1-2 months is commonly seen in such cases. In this case, patient developed this after 3 weeks of the Offending agent.
CME INDIA Learning Points
- DIGO is most commonly observed in male children and adolescents, primarily affecting the anterior gingival tissue. Its development is influenced by genetic factors, with severity varying based on the drug used. Phenytoin, cyclosporin, and nifedipine are the leading causes, with phenytoin having the highest prevalence. Approximately 50% of adults on phenytoin, 30% on cyclosporin, and 20% on nifedipine experience gingival enlargement.
- Pathophysiology of DIGO: DIGO is influenced by genetic predisposition, as not all individuals on the same drug develop gingival overgrowth. The condition arises due to inhibited cation influx, particularly sodium and calcium ions, leading to reduced folic acid uptake in gingival fibroblasts. This disrupts collagen metabolism, resulting in excessive connective tissue accumulation.
- Key Mechanisms:
- Gingival Fibroblasts & Folate Uptake: Drug-induced fibroblast activation increases glycosaminoglycan (GAG) production, while decreased intracellular folate impairs matrix metalloproteinase activation, leading to excess collagen build-up.
- Matrix Metalloproteinases (MMPs): Inhibited collagenase activation results in extracellular matrix accumulation and gingival hypertrophy.
- Inflammatory Cytokines: Elevated IL-1β and IL-6 levels promote fibroblast proliferation and collagen synthesis.
- Na+/Ca2+ Ion Flux Disruption: Anticonvulsants and calcium channel blockers reduce calcium ion uptake in fibroblasts, altering ion flux and affecting tissue homeostasis.
- Plaque & Inflammation: Drug concentration in gingival crevicular fluid exacerbates inflammation, upregulating transforming growth factor-beta 1 (TGF-β1), worsening gingival overgrowth. Plaque control is essential for management and prevention.
- Treatment of DIGO:Treatment aims to relieve discomfort, reduce inflammation and swelling, and improve cosmetic appearance. Medical management is the first-line therapy, with surgery reserved for persistent or recurrent cases.
- Medical Management
- Drug Modification: Substituting phenytoin with carbamazepine or valproic acid, using diltiazem or verapamil instead of nifedipine, and replacing cyclosporin with tacrolimus may reduce DIGO risk. Azithromycin with cyclosporin has also shown benefits.
- Plaque Control: Maintaining oral hygiene, professional cleaning, and regular scaling.
- Inflammation Control: NSAIDs, antibiotics, topical antifungals (e.g., nystatin), and folate supplementation.
- Observation Period: A waiting period of 6–12 months after stopping the causative drug is recommended before considering surgery.
- Surgical Management
- Gingivectomy and Periodontal Flap Surgery for severe cases.
- Electrocautery for fragile gingiva or paediatric cases.
- Laser Surgery (CO₂ Laser, 10600 nm) offers precise tissue removal, haemostasis, and bactericidal effects, making it superior to scalpels.
- Medical Management
CME INDIA Tail-Piece
- If the causative medication can be replaced with a drug less likely to induce gingival overgrowth, the condition may resolve with proper plaque control. However, in some cases, gingival enlargement persists despite drug substitution and good oral hygiene, necessitating surgical intervention to restore normal gingival contours.
- In 1996, Seymour et al. proposed that genetic predisposition plays a role in the development of DIGO, explaining why some individuals on the same medication develop gingival overgrowth while others do not.
References:
- Doufexi A, Mina M, Ioannidou E. Gingival overgrowth in children: epidemiology, pathogenesis, and complications. A literature review. J Periodontol. 2005 Jan;76(1):3-10.
- Seymour RA, Ellis JS, Thomason JM. Risk factors for drug-induced gingival overgrowth. J Clin Periodontol. 2000 Apr;27(4):217-23.
- Mavrogiannis M, Ellis JS, Thomason JM, Seymour RA. The management of drug-induced gingival overgrowth. J Clin Periodontol. 2006 Jun;33(6):434-9
- Trackman PC, Kantarci A. Molecular and clinical aspects of drug-induced gingival overgrowth. J Dent Res. 2015 Apr;94(4):540-6.
- Agrawal AA. Gingival enlargements: Differential diagnosis and review of literature. World J Clin Cases. 2015 Sep 16;3(9):779-88
- Nemoto E, Sugawara S, Takada H, Shoji S, Horiuch H. Increase of CD26/dipeptidyl peptidase IV expression on human gingival fibroblasts upon stimulation with cytokines and bacterial components. Infect Immun. 1999 Dec;67(12):6225-33. doi: 10.1128/IAI.67.12.6225-6233.1999. PMID: 10569731; PMCID: PMC97023.
- Gheonea TC, Șurlin P, Nicolae FM, Gheorghe DN, Popescu DM, Rogoveanu I. Dipeptidyl-Peptidase-4 and Glucagon-like-Peptide-1, a Link in the Connection between Periodontitis and Diabetes Mellitus-What Do We Know So Far?-A Scoping Review. J Clin Med. 2024 Feb 4;13(3):903. doi: 10.3390/jcm13030903. PMID: 38337597; PMCID: PMC10856081.
Discover CME INDIA:

- Explore CME INDIA Repository
- Examine CME INDIA Case Study
- Read History Today in Medicine
- Register for Future CMEs