CME INDIA Presentation by Dr. N. K. Singh, Director, Diabetes & Heart Reserch Centre, Dhanbad, Dr. Akashkumar Singh, Consultant Physician, Vadodara, Dr. Hemen Vithlani, Senior Radiologist, Vadodara.
1. Introduction
Positron Emission Tomography–Computed Tomography (PET-CT) has become a cornerstone of precision diagnostics in oncology, neurology, cardiology, and infectious diseases. By combining molecular imaging with anatomical details, PET-CT offers unmatched insight into disease processes. This updated national guidance integrates key clinical indications, tracer selection, costs, patient preparation, safety issues, structured reporting, and future directions for internists, physicians, diabetologists, and subspecialists.
2. Clinical Conditions Where PET-CT Should Be Considered
a. Common Indications
- Oncology:
- Staging and restaging of lung, breast, colorectal, head and neck cancers, and lymphomas.
- Evaluation of metastases (especially bone, liver, and brain).
- Monitoring treatment response and detecting recurrence.
- Neurology:
- Alzheimer’s disease (amyloid and tau imaging).
- Parkinson’s disease and atypical parkinsonian syndromes.
- Epilepsy (localizing seizure foci in refractory cases).
- Cardiology:
- Myocardial perfusion (Rubidium-82, N-13 ammonia PET).
- Viability studies (hibernating myocardium using FDG).
- Cardiac sarcoidosis, myocarditis, and inflammatory conditions.
- Infectious/Inflammatory Conditions:
- Fever of unknown origin (FUO).
- Vasculitis and large vessel inflammation.
- Prosthetic joint infections or cardiac device infections.
b. Unusual but Relevant Scenarios
- Neuroendocrine Tumors (NETs): Ga-68 DOTATATE PET-CT is now standard for detection and staging.
- Prostate Neuroendocrine Tumors (PNETs): May benefit from specialized tracers such as Ga-68 DOTATATE or F-18 FDOPA.
- Rare Cancers: Sarcomas, melanoma, and less frequent malignancies where PET-CT aids in metastatic survey.
- Amyloid PET: Useful in atypical dementias and research into Alzheimer’s disease.
3. Types of PET-CT and Their Clinical Use
- F-18 FDG PET-CT: Oncology (most solid tumors, lymphomas), infections, inflammatory disorders.
- Ga-68 PSMA PET-CT: Prostate cancer (initial staging, recurrence, metastases).
- Ga-68 DOTATATE PET-CT: Neuroendocrine tumors.
- F-18 Amyloid PET: Alzheimer’s disease diagnosis.
- F-18 NaF PET: Bone metastasis imaging.
- F-18 DOPA PET: Movement disorders, pheochromocytoma, and PNETs.
4. Cost of PET-CT
- Abroad (USA/Europe): Approximately USD $1,000 – $5,000, depending on tracer and center.
- India: Approximately ₹20,000 – ₹40,000 per scan, with specialized tracers (PSMA, DOTATATE) sometimes costing more.
- Reimbursement: Insurance coverage is variable. Many government schemes and private insurers in India cover FDG PET for oncology indications but may restrict approval for newer tracers.
5. Patient Preparation and Precautions
a. Laboratory Tests Before PET-CT
- Blood glucose level: Mandatory before FDG PET. Ideal fasting blood glucose < 150 mg/dl.
- Renal function tests (serum creatinine, eGFR): Essential if IV contrast for CT is planned.
- Complete blood count and LFTs: Occasionally required based on clinical context.
b. Fasting Guidelines
- FDG-PET: Patients should fast for 4–6 hours before the scan. Water is permitted.
- Sugar restriction: Avoid sweets, glucose, or carbohydrate-rich drinks for at least 6 hours. High glucose levels or recent sugar intake can cause false-negative scans due to competitive inhibition of FDG uptake by normal tissues.
c. Renal Function Impairment
- If renal function is impaired, PET can be done without IV contrast for CT. The CT will serve for anatomical localization but not for full diagnostic evaluation.
- Interpretation: Lesion localization remains accurate, but small or subtle structural abnormalities may be less clear compared to contrast-enhanced CT.
d. Other Precautions
- Hydration: Encourage oral hydration before and after the scan to aid tracer clearance.
- Diabetic patients: Adjust insulin/medication timing; hypoglycemia should be avoided.
- Pregnancy: Contraindicated unless benefits outweigh risks; thorough counseling required.
6. Procedure of PET-CT (For Physician Knowledge)
- Tracer injection: Patient receives a small dose of radiotracer (commonly FDG).
- Uptake period: Patient rests quietly for 45–60 minutes while tracer distributes in the body.
- Scan acquisition: Patient lies on the PET-CT table. First, a low-dose CT is performed (with or without contrast), followed by PET emission imaging.
- Image reconstruction: Functional PET images are fused with anatomical CT images.
- Duration: Entire procedure takes 2–3 hours including waiting period; scanning itself lasts 20–30 minutes.
7. Radiation Dose and Safety
- Typical PET-CT radiation dose: 7–15 mSv, comparable to a diagnostic CT.
- Total-body PET scanners reduce exposure while enhancing sensitivity.
- Cumulative exposure should be monitored in oncology patients undergoing repeated scans.
- Special Populations:
- Pediatric patients: Prefer PET/MRI for reduced radiation.
- Elderly/frail patients: Consider mobility, sedation needs, and comorbidities.
- Immunocompromised patients: Be cautious of false positives from infections/inflammation.
8. Structured Reporting Standards
- Oncology: Use PERCIST (PET Response Criteria in Solid Tumors) for therapy response.
- SUV values: Provide standardized uptake values with interpretation context.
- Neurology & Cardiology: Structured templates enhance reproducibility.
9. Importance of Early Collaboration with Nuclear Medicine Specialists
- Protocol Optimization: Early communication with the reporting radiologist/nuclear medicine physician ensures the most appropriate tracer is selected and scanning parameters are tailored to the clinical question.
- Interpretation Accuracy: Clinical context and history shared beforehand reduce false positives/negatives.
- Multidisciplinary Integration: Participation in tumor boards and joint discussions improves treatment planning and outcomes.
Diagnostic Performance
| Clinical Context | Sensitivity | Specificity | Notes |
| Lung cancer staging | 85–95% | 80–90% | False positives in TB, sarcoidosis |
| Lymphoma response | >90% | >85% | Useful for therapy adaptation |
| FUO/infection | ~80% | ~70% | Infections/inflammation mimic malignancy |
| Dementia (Amyloid PET) | ~88% | ~85% | Research to routine transition |
10. Practical Guidance for Physicians
- Select appropriate tracer based on indication.
- Always consider PET-CT in staging, metastasis detection, and FUO cases.
- Communicate clinical details clearly to the imaging team.
- Ensure laboratory tests and fasting protocols are followed.
- Consider non-contrast CT in patients with renal impairment.
- Counsel patients regarding costs, safety, and preparation.
- Leverage PET-CT findings in multidisciplinary decision-making.
- Refer to standardized reporting (PERCIST, SUV-based metrics).

11. Future Directions
- Novel tracers: Immuno-PET (PD-L1), hypoxia tracers, and mutation-specific probes.
- Theranostics: Lu-177 PSMA and other radionuclide therapies expanding in India.
- Regulatory landscape: Ongoing Indian clinical trials are expanding PET’s applications beyond oncology.
- Access: Wider adoption of PET/MRI and mobile PET units may enhance rural availability.
12. Conclusion
PET-CT has evolved from an oncology-focused tool to a versatile imaging modality in neurology, cardiology, and infectious disease management. With multiple tracers now available, its applications are broader than ever. Early discussion with nuclear medicine specialists, judicious selection of tracers, structured reporting, strict adherence to preparation protocols, and awareness of costs are essential to maximize patient benefit. PET-CT remains integral to evidence-based, patient-centered care in 2025.
CME INDIA Clinical Pearls – Take Home Messages
| Think PET-CT early – especially in oncology staging, unexplained fevers, and atypical inflammatory conditions. |
| Tracer choice matters – FDG for most tumors and infections, PSMA for prostate cancer, DOTATATE for NETs, Amyloid for dementia. |
| Discuss before you scan – protocol optimization with nuclear medicine ensures better accuracy and avoids repeat scans. |
| Lab tests first – check blood glucose before FDG PET; assess renal function if contrast-enhanced CT is planned. |
| Patient preparation is crucial – fasting for 4–6 hours, avoid sugar, hydrate well. Poor preparation compromises image quality. |
| Diabetes adjustments – uncontrolled hyperglycemia reduces FDG uptake; hypoglycemia must be avoided. |
| Renal impairment is not a barrier – PET can proceed with non-contrast CT; interpretation remains robust though CT detail is reduced. |
| Consider costs upfront – scans are 4–5 times more expensive abroad than in India; insurance coverage is variable. |
| False positives exist – infection and inflammation can mimic cancer; always correlate clinically. |
| Procedure knowledge helps – PET-CT involves tracer injection, uptake waiting, and scanning; total time ~2–3 hours. |
| Radiation awareness – typical dose 7–15 mSv; prefer PET/MRI in pediatrics. |
| Structured reporting adds clarity – PERCIST and SUV-based interpretation improve consistency. |
| Multidisciplinary approach – integration with tumor boards, cardiology rounds, and neurology meetings maximizes value. |
| Patient safety first – optimize preparation, limit radiation exposure, and counsel patients well. |
| Broader than cancer – remember PET’s role in neurology, cardiology, and infection evaluation. |
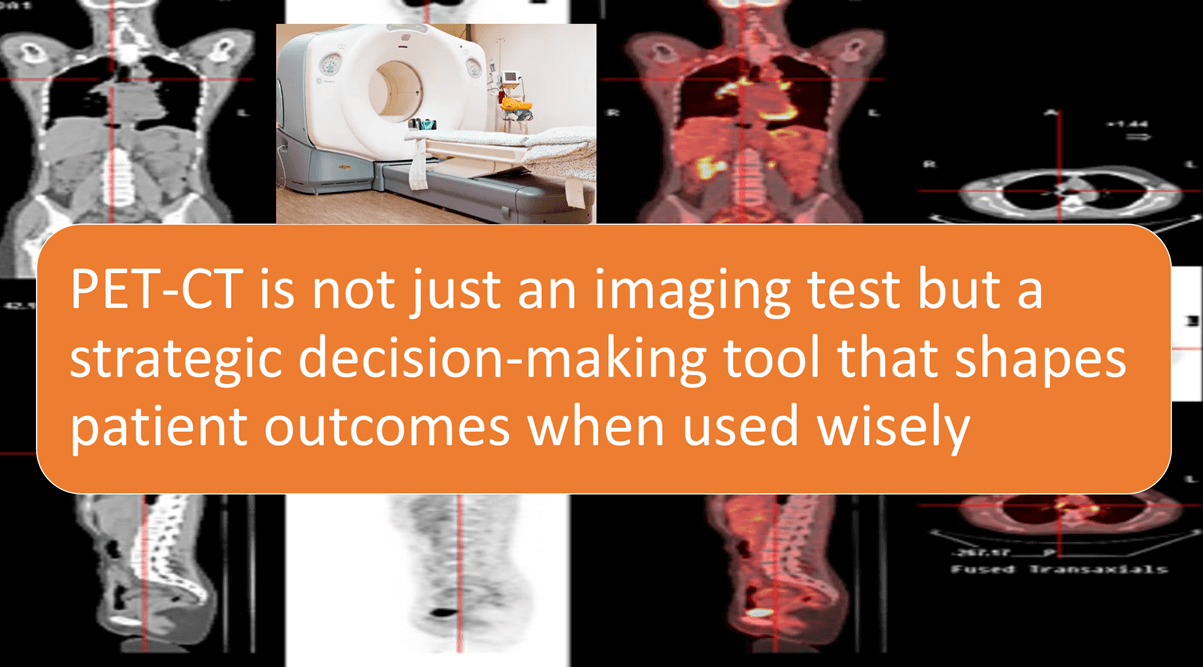
Bottom line: PET-CT is not just an imaging test but a strategic decision-making tool that shapes patient outcomes when used wisely.
References:
- Calderoni, L., Giovanella, L., & Fanti, S. (2024). Endocrinology application of molecular imaging: Current role of PET/CT. Journal of Endocrinological Investigation, 47(10), 2383–2396. https://doi.org/10.1007/s40618-024-02400-8 (SpringerLink)
- Ali, J., et al. (2024). The usefulness of FDG PET-CT in the routine staging of gastric cancer: detecting previously unidentified metastases. Indian Journal of Nuclear Medicine. [Ahead of print] (Lippincott Journals)
- Mahajan, A., et al. (2024). Indian clinical practice pre-treatment imaging guidelines for head and neck cancers: role of FDG PET-CT in detecting distant and thoracic metastasis. Clinical and Translational Radiation Oncology. [Article] (Lippincott Journals)
- Frontiers in Oncology. (2025). PSMA-based theranostics in diagnosing and treating prostate cancer: recent progress and clinical prospects. Frontiers in Oncology. [Review] https://doi.org/10.3389/fonc.2025.1655082 (Frontiers)
- Yadav, M. P., Ballal, S., Sahoo, R. K., Tripathi, M., Seth, A., & Bal, C. (2020; data referenced in more recent follow-ups) but particularly, the study “Efficacy and safety of ²²⁵Ac-PSMA-617 targeted alpha therapy in metastatic castration-resistant prostate cancer patients” as reported in Theranostics, 10(20), 9364–9377. https://doi.org/10.7150/thno.48107 (thno.org)

Discover CME INDIA

- Explore CME INDIA Repository
- Examine CME INDIA Case Study
- Read History Today in Medicine
- Register for Future CMEs