CME INDIA Presentation by Hemant Bhargav, MD, PhD; Associate Professor; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India. Suman Bista, MSc, PhD; Nishitha Jasti, BNYS, MSc, Umesh Chikkanna, MD; Shiva Kumar V, PhD; Kishore Kumar R, MD, PhD; Shivarama Varmbally, MD, DSc; S Srikanta, MD; R Nagarathna, MD; R Padmavati, MD; Govindrao Kusneniwar, MD; N K Singh, MD; B N Gangadhar, MD; K N Manohar, MD.
Yoga Outsmarts Diabetes
Background and Context
- T2DM constitutes one of the major global public-health challenges of our era. The International Diabetes Federation (IDF) estimates that over 9 % of adults worldwide have diabetes (predominantly T2DM), and projections suggest significant further increases by 2045. India in particular bears a major burden: recent surveys show ~11–12 % diabetes prevalence among adults aged ≥20 and ~15 % pre-diabetes, with a high rate of abdominal obesity (~39.5 %) in some states. In this scenario, lifestyle‐based interventions (diet, physical activity, stress reduction) have rightly become a cornerstone of diabetes prevention and management.
- Yoga — a traditional Indian holistic practice combining physical postures (asanas), breathing exercises (pranayama), meditation and lifestyle guidance — is of special interest in the Indian context, both culturally and practically.
- Meta‐analyses of 30+ randomised trials suggest that yoga, when added to usual care, improves glycaemic control and risk‐factors for T2DM. Yet many of these studies have limitations: small sample-size, short duration (<6 months), lack of active control groups (e.g., aerobic exercise) and limited mechanistic biomarkers. Thus the field has been calling for longer, better‐designed RCTs with active comparators and follow‐up beyond six months. The Bhargav et al. trial explicitly addresses this gap.
Abstract
A year-long, two-arm, assessor-blinded randomized controlled trial evaluated the long-term effects of a yoga-based lifestyle (YBL) intervention versus matched physical exercise and health education (PHE) in adults with type 2 diabetes mellitus (T2DM). A total of 162 participants (mean age 53.3 ± 9 years; mean diabetes duration 6.7 years) from Bengaluru, India, were randomized 1:1 to receive standard diabetes care plus YBL or PHE. The YBL group underwent 4 weeks of supervised daily yoga (1 h/day, 5 days/week), followed by 11 months of tele-supervised practice with weekly counselling; the PHE group performed matched exercise sessions with health education. Outcomes were assessed at baseline, 6 months, and 12 months.
The primary outcome was glycaemic control (HbA1c, fasting and postprandial glucose), and secondary outcomes included anthropometry (BMI, waist–hip ratio), psychological states (DASS-42), novel biomarkers (thermal and GDV imaging), and medication use.
At 12 months, both groups showed improved HbA1c and waist–hip ratio, but YBL produced greater HbA1c reduction (–1.25 %, p < 0.01) and better postprandial glucose, BMI, and depression scores than PHE. Thermal imaging parameters correlated negatively with HbA1c, and GDV indices (organ, adrenal, cerebral balance) improved significantly in the YBL group. Medication use decreased more in YBL participants.
Of 160 randomized, 91 completed 12 months (48 YBL, 43 PHE); attrition (~43 %) was mainly due to time constraints. The study concludes that a yoga-based lifestyle intervention provides superior long-term benefits over conventional exercise and education in improving glycaemic control, psychological well-being, and novel physiological biomarkers in T2DM management.
Strengths
- Active Comparator. Unlike many yoga trials that compare with usual‐care or no‐intervention, this study used a matched physical-exercise + health-education arm. This strengthens the claim that yoga adds benefit over exercise alone.
- Long‐term Duration (12 months). Many previous trials were short (weeks to 3-6 months); here the 12-month follow-up enhances clinical relevance and sustainability.
- Comprehensive Outcomes. Beyond glycaemic and anthropometric outcomes, the study incorporated psychological variables, medication‐use, sophisticated imaging biomarkers (thermal, GDV) — giving a multidimensional perspective on intervention effects.
- Blinded Assessors & Intent‐to‐Treat Analyses. The study used assessor‐blinding and intention‐to-treat (with per‐protocol) analyses, which add methodological rigour.
- Cultural Adaptation. The yoga intervention is regionally appropriate for Indian adults with T2DM, potentially increasing acceptability and real-world applicability.
Limitations and Caveats
- Drop‐out Rate & Attrition Bias. Only 91 of the 160 randomised completed 12 months (~57 %). This attrition is relatively high; reasons such as time constraints may bias results (e.g., those remaining may be more motivated). The per‐protocol completers may differ systematically from drop-outs.
- Generalizability. The sample is from a tertiary care setting in Bengaluru; results may not generalise to less‐resourced, rural, or non-Indian settings. Moreover, participants had relatively moderate T2DM duration (~6.7 yrs) and were smartphone/internet‐capable (tele-supervision); this may limit applicability in low‐tech settings.
- Blinding & Behavioural Bias. While outcome assessors were blinded, participants necessarily knew their allocation (yoga vs exercise). This opens potential for expectation/placebo effects. Moreover, the weekly counselling in the yoga arm may have added behavioural support beyond the exercise arm.
- Control Arm Content & Intensity. The PHE arm is described as matched for metabolic equivalents, but the exact intensity, fidelity of exercise, and supervision levels may differ from yoga (especially tele-supervision vs in-person). Differential supervision/adherence could amplify effect size.
- Mechanistic Interpretation of Novel Biomarkers. Thermal imaging and GDV are intriguing but relatively novel and less well-validated in large T2DM trials. While correlations with HbA1c are reported, causality remains speculative.
- Medication Adjustment. Participants continued routine care and medications were adjusted by treating endocrinologists; while medication use scores were tracked, the potential for confounding by changes in pharmacotherapy remains.
Mechanisms: Why Might Yoga Be Better Than Exercise Alone?
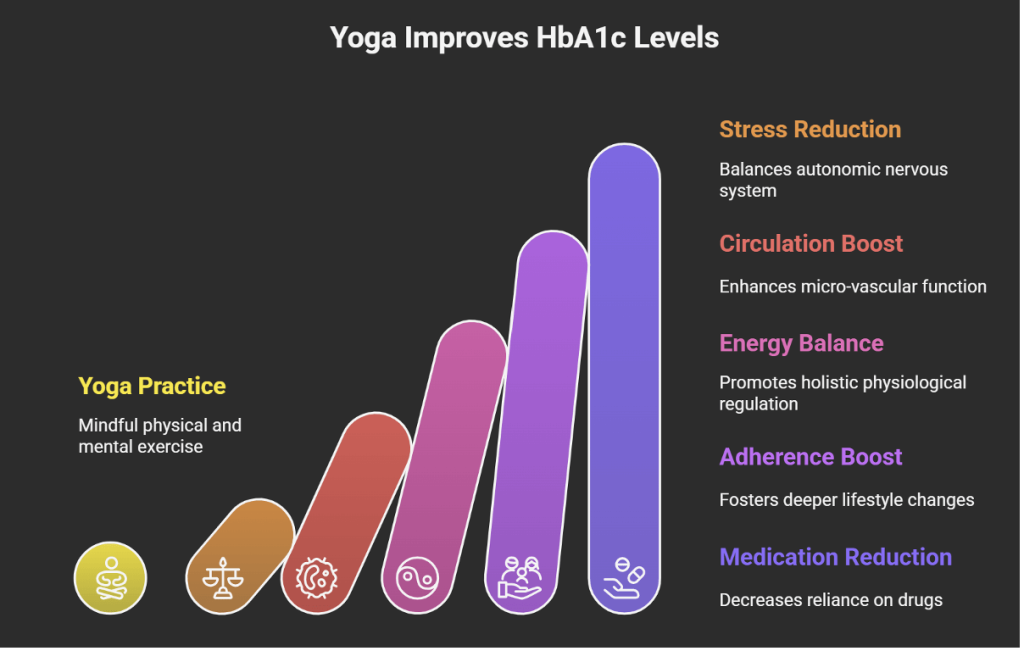
The superior effect of yoga on HbA1c (≈1.25 % greater reduction at 12 months) merits reflection on underlying mechanisms. Several plausible pathways emerge:
- Physical activity + metabolic equivalents. The yoga protocol included joint‐loosening, dynamic asanas, pranayama, and relaxation; these may broadly match moderate exercise but also include stretching, balance and breathing components that may influence autonomic and vascular function differently from conventional aerobic/strength exercise.
- Stress‐modulation / autonomic rebalancing. Yoga’s emphasis on pranayama, meditation and relaxation may better reduce sympathetic overactivity, improve parasympathetic tone, and modulate hypothalamic–pituitary–adrenal (HPA) axis activation. Chronic stress contributes to insulin resistance, impaired glucose regulation and vascular dysfunction; thus, stress-reduction may enhance glycaemic control above and beyond physical activity alone.
- Improved micro-vascular circulation / thermal regulation. The thermal‐imaging findings (negative correlations between skin temperatures in facial/ear regions and HbA1c) suggest that improved peripheral circulation, perhaps mediated via endothelial function or autonomic control, may link yoga to better glycaemia and potentially fewer diabetic complications.
- Energy/organ-balance (GDV findings). The GDV imaging indicated improvements in “organ balance,” “adrenal balance,” “cerebral cortex balance” in the yoga group. While the mechanistic underpinnings remain speculative, these findings may reflect holistic physiological regulation (bio-energetic homeostasis) rather than purely metabolic/institutional pathways.
- Behavioural adherence & lifestyle competence. The yoga intervention included weekly counselling and philosophy, which may foster deeper lifestyle behaviour change (diet, sleep, stress coping) beyond physical exercise alone. This could contribute to sustained improvements in glycaemic control and reduced medication needs.
- Medication-sparing effect. The reduction in medication‐use scores at 12 months in the yoga arm suggests that improved metabolic control was not simply due to higher pharmacologic intensification, enhancing the clinical relevance of the finding.
All of this builds a plausible case that yoga may offer added value over matched physical exercise by addressing psychosomatic, vascular, autonomic and lifestyle‐behaviour domains that contribute to T2DM pathophysiology.

Clinical and Public Health Implications
- From a clinical standpoint, the findings suggest that integrating a structured yoga-based lifestyle programme as an adjunct to standard care in T2DM patients may yield measurable benefits in glycaemic control (HbA1c), obesity/anthropometry (BMI, waist-hip ratio), psychological health (depression) and medication load. An HbA1c difference of ~1.25 % is clinically meaningful — associated with lower microvascular and macrovascular complication risk.
- From a public health viewpoint, especially in India and other South Asian settings, yoga may be a culturally acceptable, scalable lifestyle intervention. Tele-supervised delivery (as used after the first month) enhances reach and may reduce cost/resource barriers. Given the rising burden of diabetes and resource constraints, this kind of intervention could be integrated into diabetes‐care programmes, community health initiatives or insurance-reimbursed lifestyle prescriptions.
- Moreover, the results provide an impetus for guideline committees and diabetes management algorithms to consider “mind–body” interventions like yoga as a component of comprehensive lifestyle therapy — not just as niche or alternative, but as evidence‐based adjunct.
Future Directions
Replication and scaling. It is essential to replicate these findings in other settings (rural, lower‐income, non-tertiary centres), across diverse age/ethnic groups and to test sustainability beyond 12 months (2-3 years and beyond).
Mechanistic studies. The novel biomarker findings (thermal, GDV) are intriguing and warrant deeper mechanistic investigations: endothelial function (flow‐mediated dilation), autonomic indices (heart‐rate variability), inflammatory/cytokine profiles, adipokines, insulin‐sensitivity (HOMA-IR), and even epigenetic/omics approaches.
Cost-effectiveness and implementation research. For large‐scale adoption, analyses of cost, resource‐utilization, adherence strategies, tele-delivery effectiveness, and integration into existing diabetes‐care infrastructure are required. Comparative studies of yoga vs other exercise/lifestyle interventions in “real‐world” settings are important.
Tailoring & stratification. Identifying which subgroups benefit most (e.g., age, duration of T2DM, baseline control, presence of complications) will allow precision in prescribing yoga‐interventions. Dose–response studies (frequency, duration, supervision level) are also needed.
Comparative trials. Direct head-to-head trials comparing different lifestyle modalities (yoga vs aerobic/strength vs combined vs diet‐only) with long-term follow-up and standardised endpoints (HbA1c, complications, mortality) would further clarify the relative benefit.
Integration with diet and other lifestyle components. While the study focused on yoga vs exercise, future research might integrate yoga with tailored diet (e.g., low‐glycaemic index, Mediterranean style), sleep hygiene, stress‐management and digital feedback to optimise outcomes.

CME INDIA Learning Points
- The Bhargav et al. study provides a strong and timely addition to the literature on yoga‐based lifestyle interventions for T2DM. Its strengths — active comparator, year‐long follow-up, multidimensional outcomes — elevate it above many earlier trials. The observed ~1.25 % greater reduction in HbA1c, along with improvements in BMI, depression and medication usage, suggest that yoga offers meaningful added value over exercise plus health education alone.
- That said, limitations (attrition, generalisability, blinding) mean we should interpret findings with caution and demand further replication. The mechanistic biomarker findings are provocative but remain exploratory. Clinically, however, the evidence is strong enough to justify the integration of structured yoga programmes into comprehensive diabetes‐care pathways—especially in culture‐appropriate contexts like India.
- In public health terms, given the rising global diabetes burden and the need for scalable, acceptable interventions, yoga may represent a cost-effective adjunct in the armamentarium of lifestyle therapy. Going forward, implementation research, long‐term follow-up, cost-effectiveness data and mechanistic elucidation will strengthen the case further.
- In sum: for adults with T2DM, structured yoga-based lifestyle intervention appears to offer advantages over standard exercise programmes in terms of glycaemic control, psychological well-being and lifestyle behaviour. It is time for clinicians, diabetes‐care programmes and policy-makers to recognise and test the integration of yoga into standard care — while researchers deepen understanding of how and for whom it works best.
CME INDIA Tail Piece
Link- https://pubmed.ncbi.nlm.nih.gov/41118624/
Authors:
Controlled Trial
Hemant Bhargav 1 , Suman Bista 2 , Nishitha Jasti 3 , Umesh Chikkanna 3 , Shiva Kumar V 4 , Kishore Kumar R 5 , Shivarama Varmbally 6 , S Srikanta 7 , R Nagarathna 8 , R Padmavati 9 , Govindrao Kusneniwar10 , N K Singh 11 , B N Gangadhar 12 , K N Manohar 13
Affiliations
- 1 Associate Professor; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India.
- 2 PhD Scholar, School of Yoga and Physical Sciences, S-VYASA Yoga University, Bangalore, India; Junior Research Fellow, Department of Integrative Medicine, NIMHANS, Bengaluru, India.
- 3 Scientist C; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India.
- 4 Scientist-D; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India.
- 5 Professor and Head; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India.
- 6 Professor of Psychiatry; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India.
- 7 Medical Director and Consultant Endocrinologist, Samatvam Endocrinology Diabetes Center, Bangalore, India.
- 8 Medical Director, Swami Vivekananda Yoga Anusandhana Samsthana (S-VYASA) University, Bengaluru, India.
- 9 Professor of Psychiatry and Director, Schizophrenia Research Foundation (SCARF), Chennai, India.
- 10 Additional Professor of Community and Family Medicine, Department of Community and Family Medicine, AIIMS Bibinagar, India.
- 11 Director at Diabetes and Heart Research Centre, Dhanbad, Jharkhand, India.
- 12 Director; Department of Integrative Medicine, National Institute of Mental Health & Neurosciences (NIMHANS), Bangalore, India.
- 13 Consultant Internal Medicine and Diabetologist, Manipal Hospitals, Bengaluru, India.
References:
- Bhargav H, Bista S, Jasti N, et al. Effect of a Year-long Yoga-Based Lifestyle Intervention on Glycaemic Control, Body Weight, Psychological Health, and Imaging Biomarkers in Adults with Type 2 Diabetes: A Randomised Controlled Trial. Adv Mind Body Med. E-pub ahead of print. 2025.
- Raghuram N, Ram S, Majumdar V, et al. Effectiveness of a Yoga-Based Lifestyle Protocol (YLP) in Preventing Diabetes in a High-Risk Indian Cohort: The Niyantrita Madhumeha Bharat Abhiyan (NMB) Trial. Front Endocrinol 2021;12:664657. (Frontiers)
- Kaur N, Majumdar V, Nagarathna R, Malik N, Anand A, Nagendra HR. Diabetic Yoga Protocol Improves Glycaemic, Anthropometric and Lipid Levels in High-Risk Individuals for Diabetes: RCT from Northern India. Diabetol Metab Syndr 2021;13:149. (dmsjournal.biomedcentral.com)

Discover CME INDIA

- Explore CME INDIA Repository
- Examine CME INDIA Case Study
- Read History Today in Medicine
- Register for Future CMEs

