CME INDIA Presentation by Dr. S. K. Gupta, MBBS, MD (Med), CFM (France), Senior Consultant Physician, Max Hosp., Delhi.
Pandemic of AMR (Antimicrobial resistance)
- The menace of antimicrobial resistance (AMR) has the potential to snowball into a global crisis with pandemic-like effects. AMR does not spread like infectious diseases caused by a single pathogen, such as COVID-19; rather, it is a broad issue affecting the effectiveness of antibiotics against a wide range of bacteria. Here’s why the global threat of AMR can be considered as severe as a pandemic:
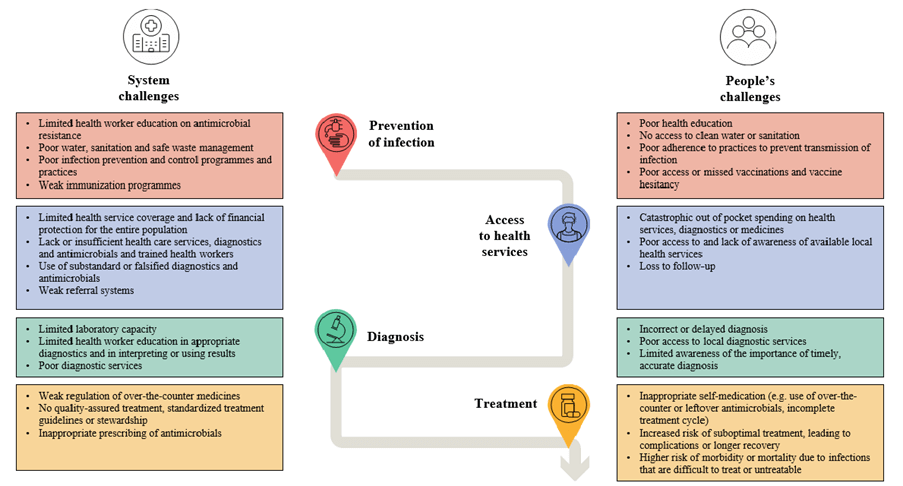
Figure: System and people’s challenges for antimicrobial resistance. Courtsey: WHO, WHO strategic and operational priorities to address drug-resistant bacterial infections in the human health sector,2025–2035 EXECUTIVE BOARD EB154/13154th session 21 December 2023.Provisional agenda item 13
Widespread Impact
- AMR can lead to infections that are resistant to current treatment options, rendering common infections, such as pneumonia, urinary tract infections, and sepsis, difficult or even impossible to treat. These resistant infections can affect anyone, of any age, in any country.
Increased Mortality and Morbidity
- As bacteria evolve to resist the effects of antibiotics, we face the possibility of returning to a time when even minor infections could cause severe complications or death. This would increase both mortality and morbidity, straining global healthcare systems.
Economic Burden
- The economic impact of AMR is substantial. It leads to longer hospital stays, higher medical costs, and greater healthcare resource utilization. The productivity loss due to increased sickness and mortality also contributes to economic strain.
Spread and Transmission
- Resistant bacteria can spread between individuals and across borders with ease, particularly in our highly interconnected world. They can also move between humans, animals, and the environment, complicating efforts to control their spread.
Global Health Security Threat
- AMR undermines advances in modern medicine, including the ability to perform complex surgeries and cancer chemotherapy, which depend on effective antibiotics to manage infections. The erosion of these capabilities poses a severe threat to global health security.
Strategies to Manage AMR
Efforts to manage AMR include promoting antimicrobial stewardship to prevent overuse and misuse of antibiotics, enhancing surveillance to monitor AMR patterns, and increasing awareness through public health campaigns. Research and development also play a crucial role, focusing on new drugs and improving diagnostic tools to ensure effective treatment decisions.
1.Research into antimicrobial resistance (AMR)
It encompasses a broad range of disciplines, from molecular biology and epidemiology to public health and policy studies. Here are some notable examples of recent research efforts addressing different aspects of AMR:
Development of New Antibiotics and Treatments
Teixobactin: Discovered as part of a novel method for growing previously unculturable bacteria, teixobactin is an antibiotic that has been shown to be effective against a range of pathogenic bacteria without developing resistance.
1a. Phage Therapy
Phage therapy involves using bacteriophages—viruses that infect and kill bacteria—to treat bacterial infections, especially those resistant to antibiotics.
Intralytix and Pherecydes Pharma: These companies have been pioneers in clinical applications of phage therapy. They have developed phage preparations for use against multi-drug-resistant bacterial infections, such as those caused by Staphylococcus aureus and Pseudomonas aeruginosa.
Cystic Fibrosis Treatment: A notable case study involved a teenage patient with cystic fibrosis who was treated with a cocktail of bacteriophages in 2019. The phages were specifically chosen to combat a resistant Mycobacterium abscessus lung infection. This treatment was personalized and demonstrated significant improvement in the patient’s health.
1b. Antibiotic Adjuvants
Adjuvants are compounds that enhance the efficacy of antibiotics, helping to overcome resistance mechanisms.
Efflux Pump Inhibitors: One strategy to combat resistance is to use inhibitors of efflux pumps, which many resistant bacteria use to pump antibiotics out of their cells. Compounds like verapamil have been studied for their ability to enhance the effectiveness of antibiotics against resistant strains by inhibiting these pumps.
Beta-lactamase Inhibitors: Clavulanic acid, sulbactam, and tazobactam are used in combination with beta-lactam antibiotics to inhibit the beta-lactamase enzyme, which many bacteria produce to degrade beta-lactam antibiotics. These combinations are well-established in clinical use, with Augmentin (amoxicillin/clavulanate) being a prominent example.
1c. Drug Combinations
Combining drugs can target different pathways in bacteria or prevent the activation of resistance mechanisms.
Polymyxin B and Rifampicin: This combination has been used to treat infections caused by carbapenem-resistant Acinetobacter baumannii. The combination exploits synergistic effects that can enhance bacterial killing and reduce the likelihood of resistance development.
Piperacillin/Tazobactam: This combination is used to treat a wide range of infections, including those caused by Pseudomonas aeruginosa. Tazobactam inhibits beta-lactamase, enhancing the efficacy of piperacillin against resistant strains.
Implementation in Clinical Settings
While these therapies offer promising alternatives or complements to traditional antibiotics, their implementation in clinical settings often requires careful consideration of specific bacterial strains, resistance profiles, and individual patient conditions. Moreover, regulatory approval processes can be complex due to the specificity and novelty of these treatments.
2. Rapid Diagnostics Development
Point-of-Care Testing Tools: Rapid diagnostic tools that can quickly determine the bacterial strain and its susceptibility to antibiotics can significantly improve the use of appropriate therapies and reduce the misuse of antibiotics. Recent advancements include CRISPR-based diagnostics that offer high specificity and speed.
3. Surveillance and Epidemiological Studies
- Global Surveillance Networks: Projects like the Global Antimicrobial Resistance Surveillance System (GLASS), initiated by WHO, focus on standardizing the collection, analysis, and sharing of data related to AMR worldwide.
- Environmental Surveillance: Research into the environmental spread of AMR, such as studies tracking the presence of resistant bacteria in wastewater, helps in understanding and mitigating the environmental transmission routes of AMR.
4. Socioeconomic and Policy Research
- Cost-Effectiveness Analyses: Economic studies assess the cost-effectiveness of interventions like stewardship programs and stricter regulations. These analyses help in understanding the economic burden of AMR and the benefits of various control strategies.
- Policy and Implementation Studies: Research on the impact of national action plans and policies on AMR trends helps in shaping effective legislation and health interventions globally.
5. Vaccine Development
- Preventive Vaccines: Developing vaccines against bacteria known to cause serious infections can reduce the incidence of these infections and consequently lower the use of antibiotics, indirectly combating AMR. Research in this area includes vaccines for organisms like Staphylococcus aureus and Streptococcus pneumoniae.
Countries Most Affected by AMR
Though Antimicrobial resistance (AMR) is a global issue affecting both high-income and low- and middle-income countries (LMICs). However, the impact and responses vary significantly across regions.
Low and Middle-Income Countries (LMICs):
These nations often bear the brunt of AMR due to several factors:
- High burden of infectious diseases: Higher prevalence of infections increases the use of antimicrobials, which can lead to resistance.
- Lack of regulation and oversight: In many LMICs, antimicrobials can be purchased without prescription, leading to misuse.
- Limited healthcare infrastructure: Insufficient healthcare facilities and lack of proper sanitation can lead to the spread of resistant infections.
Countries like India, some parts of Africa (such as South Africa and Nigeria), and Southeast Asian nations (like Thailand and Vietnam) are particularly highlighted in global AMR discussions due to their high rates of drug-resistant infections.
Countries Effectively Working to Prevent AMR
Sweden and the Netherlands: These countries are often cited as models in AMR stewardship. They have comprehensive national action plans that include:
- Strict regulations: on antibiotic prescription.
- Robust surveillance systems to monitor AMR trends.
- Public awareness campaigns to educate about the prudent use of antibiotics.
United Kingdom: The UK has been a leader in raising global awareness about AMR. It has implemented stringent antimicrobial stewardship programs and invested in research and development.
Australia and Canada: These nations have also taken significant steps in establishing strong surveillance systems and regulatory frameworks to control the use and distribution of antibiotics.
Global Initiatives
- At the international level, the World Health Organization (WHO), in collaboration with the Food and Agriculture Organization (FAO) and the World Organisation for Animal Health (OIE), promotes a One Health approach to address AMR across human, animal, and environmental health sectors globally. This approach helps in forming policies that are effective across all borders and sectors.
Key initiatives by WHO includes:
- Global Action Plan on AMR: Launched in 2015, this plan aims to ensure the prevention and treatment of infectious diseases with safe and effective medicines.
Challenges in Response
- The global response to AMR is hampered by several factors, including inadequate surveillance, slow development of new antibiotics, and insufficient global coordination. Unlike a typical infectious disease pandemic, which might be addressed with a vaccine or focused public health interventions, combating AMR requires sustained, multifaceted strategies involving healthcare, agriculture, and environmental policies.
Impact and Future Directions
- AMR has profound implications for global health security, economic stability, and healthcare practices. Countries heavily burdened by AMR, particularly in low- and middle-income regions, face significant challenges due to inadequate healthcare infrastructure and lack of regulatory frameworks. Conversely, nations with comprehensive AMR strategies showcase the potential of targeted action and innovation in mitigating this crisis.
Conclusion
- In summary, while AMR does not spread in the traditional sense of a pandemic, its widespread impact, ability to affect global health security, and the challenges it presents in management and containment mean that its potential threat is comparable to that of a pandemic. While some countries have made significant progress, AMR remains a significant challenge that necessitates continued global attention and action.
- The battle against AMR is complex and ongoing, necessitating continued innovation, collaboration, and vigilance. The integration of new treatment modalities such as phage therapy and drug combinations with robust policy frameworks and international cooperation holds the key to sustaining the efficacy of antimicrobial drugs and securing global health.
- These research efforts are crucial in combating AMR, and they involve an international network of universities, research institutes, healthcare facilities, and governments, each contributing towards a global strategy to manage and mitigate this threat.
- Efforts to combat AMR require both national and international collaboration, focusing on regulation, education, and innovation.
CME INDIA Learning Points
To address antimicrobial-resistant threats, we need to:
| 1. Strengthen the detection of antimicrobial resistance. |
| 2. Enhance efforts to slow the emergence and spread of resistance. |
| 3. Improve the use and reporting of antibiotics and antifungals. |
| 4. Advance the development of rapid diagnostics for resistant pathogens. |
| 5. Enhance infection control measures. |
| 6. Accelerate research on new antibiotics, antifungals, therapeutics, and vaccines. |
Further Reading:
- https://apps.who.int/gb/ebwha/pdf_files/EB154/B154_13-en.pdf
- Ranjalkar J, Chandy SJ. India’s National Action Plan for antimicrobial resistance – An overview of the context, status, and way ahead. J Family Med Prim Care. 2019 Jun;8(6):1828-1834. doi: 10.4103/jfmpc.jfmpc_275_19. PMID: 31334140; PMCID: PMC6618210.
- https://www.cdc.gov/antimicrobial-resistance/programs/AR-actions-events.html

Discover CME INDIA

- Explore CME INDIA Repository
- Examine CME INDIA Case Study
- Read History Today in Medicine
- Register for Future CMEs

