CME INDIA Presentation by Dr. Shaibal Guha, M.D., Consultant Physician, Associate Professor, Dept. of Medicine, Netaji Subhas Medical College, Director, Positive Health Centre, Patna.
Based on a presentation at RSSDI-Bihar conference at Darbhanga on 16/06/2024.

It matters to know the intricacies of travel and diabetes
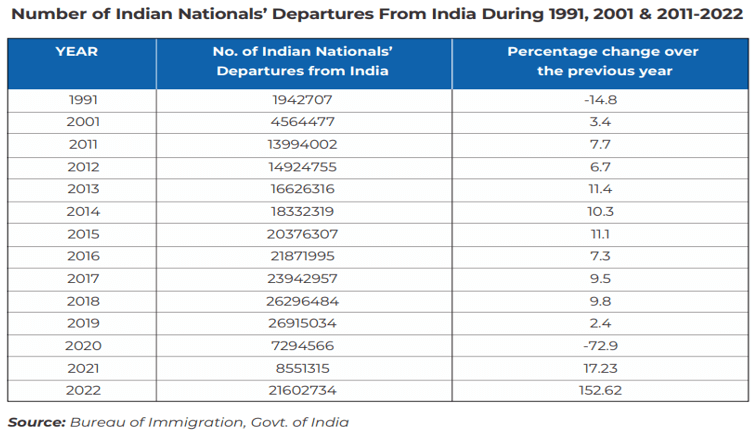
- There is an exponential rise of international travel by Indians.
- Travelling with diabetes means there are a few more things to think about before you set off.
- But living with diabetes shouldn’t be a barrier to taking trips or holidays at home or abroad.
Issues of Concern
- Pre-travel preparation
- At the airport
- During the flight/ journey
- At the destination
Instruct Patients to Plan Ahead
- Travel Insurance: Ensure your travel insurance covers pre-existing medical conditions.
- Health Advisory: Check health information and advisories specific to your destination country.
- Doctor Consultation: Meet with your doctor a few weeks before your trip to discuss any concerns, get recommendations, update immunizations, and obtain extra prescriptions if needed.
- Airline/Cruise Ship Preparations: Contact your airline or cruise ship in advance to arrange for special meals and proper insulin storage.
- Airport Guidelines: Familiarize yourself with your airport’s regulations for carrying medications, insulin, syringes, insulin pumps and supplies, lancing devices, blood glucose meters and supplies, and food for treating low blood sugar.
- Medical ID: Wear a medical ID that indicates your diabetes type.
To Do List
- Keep all your medicine, insulin, syringes, meters, test strips, pump supplies—everything you need—on you at all times.
- Make lists of important information: your doctor’s contact details, the medications you take, and emergency instructions.
- Ensure your diabetes testing supplies, equipment, and medicines are in their original packaging with prescription labels clearly visible.
- Learn key phrases in the local language, such as “I have diabetes” and “Where is the clinic or hospital?” Also, find the address of the nearest hospital.
Hand luggage – pack more, not less!
- All diabetes medications.
- Diabetes supplies, including sensors and spare devices.
- Diabetes identity card or wristband.
- A letter from your doctor detailing your diabetes and treatment, including information about your insulin pump, CGM, or flash glucose monitor.
- A prescription sheets.
- Hypo treatments and extra snacks (nuts, fruit, sandwich) in case of delays.
- If possible, split your medications between separate bags. For example, if you’re traveling with a partner or friend, share the medications between your bags to mitigate the risk of losing something.
Issues In Transit: At the Airport
Flying with an insulin pump, CGM or Freestyle Libre
- Look up the manufacturer’s advice on flying with your specific device.
- Insulin pumps, CGMs, and flash glucose sensors are all safe for use during air travel and can be connected via Bluetooth.
- If you use a CGM, insulin pump, or Freestyle Libre, security staff may request evidence that you need to use one, so you’ll need a letter from your doctor.
- Print out a Medical Device Awareness Card from the Civil Aviation Authority website. While not essential, this card can make things easier by outlining the screening rules for medical devices.
Can CGMs, insulin pumps and Freestyle Libre sensors go through airport security scanners?

Organize medication with your healthcare team
- Travel Letter: Obtain a letter that mentions you have diabetes and need to carry medical supplies. It should detail your medications, including any that need to be in containers over 100 ml, and list any devices you use.
- Prescriptions and Supplies: Ask your healthcare team for prescriptions for extra insulin, other diabetes medications, devices, additional supplies, and manual equipment. Plan to take twice the amount of medication and supplies you typically need.
- Insulin and Medication Adjustment: Seek advice on adjusting your insulin dose or insulin pump settings for long-haul flights, and inquire about any extra medication needed if crossing time zones.
- Prescription Copies: Keep copies of your recent prescriptions in each of your bags.
In Transit: during the journey
Issues during the journey
- Less Control Over Meals: Challenges with timing, food selection, and availability.
- Less Control Over Activity Levels: Difficulty maintaining regular activity routines.
- Acute Travel-Related Illness and Correcting Hypos: Managing sudden illnesses and low blood sugar episodes.
- Medicines or Supplies Lost/Depleted: Risk of losing or running out of medications or supplies.
- Insulin Storage: Ensuring proper storage conditions for insulin.
- Changing Time Zones: Adjusting insulin doses and medication schedules when crossing time zones.
- Retinopathy and Altitude: Impact of high altitude on diabetic retinopathy.
- Diabetic Foot Care: Special precautions for foot care while traveling.
- Altitude Effects on Glucometers and Insulin Pumps: Older glucometers may be affected by altitude changes.
- Increased Insulin Absorption in Hot Climates: Hot climates can increase blood flow to the skin and subcutaneous tissues, leading to higher insulin absorption.
Precautions onboard
- Carry Snacks and Treatments: Have glucose tablets, gels, or candy for hypoglycaemia and snacks like breakfast bars, crackers, or trail mix for missed or delayed meals.
- Special Meal Requests: Request meals that are low in sugar, fat, and cholesterol.
- Avoid Prolonged Sitting: Stand up, stretch, or walk around for a few minutes every hour.
- Stay Hydrated: Drink non-alcoholic, caffeine-free beverages to keep hydrated.
- Snacks on Long Flights: You may need snacks between meals and at bedtime during long flights.
- Timing Insulin Injections: Do not take pre-meal insulin until your meal is in front of you.
- Pressure Equalization: Airplane cabins are pressurized. Before using a syringe in flight, remove and replace the plunger to equalize pressure.
- Watch Time Management: Keep your wristwatch set to the departure city’s time to remember when to take insulin. Change your watch to local time the morning after arriving at your destination.
Standby antibiotics
- Treat traveller’s diarrhea
- Treat skin and soft tissue infections
- Macrolides, oints
- Diabetic foot infections
- Usually, polymicrobial
- Clavulinate, Cipro + metronidazole
- Treat vaginal candidiasis
- Fluconazole
At the destination
Travel to the tropics
- Protect Your Skin: Wear clothes that cover your skin and use sunscreen with SPF 30 or higher, ensuring it provides UV-A and UV-B protection. Choose sunglasses with a UV400 label.
- Foot Care: If you have neuropathy, protect your feet by wearing socks, applying sunscreen, and using well-fitting sandals on the beach to avoid burns from hot sand.
- Monitor Glucose Levels: Check your glucose levels more frequently than usual, as you’ll likely be walking more and trying new foods.
- Insulin Storage: Insulin damaged by heat may turn brown or cloudy. Store it in a hotel fridge or a cool bag, ensuring it does not freeze.
Sunbathing can indeed affect blood sugar levels for several reasons. Here’s how:
- Inactivity and Insulin Sensitivity: Sunbathing often involves prolonged periods of inactivity, which can lead to reduced insulin sensitivity. When you’re inactive, your muscles don’t need as much glucose, potentially causing blood sugar levels to rise. This is because insulin, which helps transport glucose from the bloodstream into cells, may not work as effectively when you’re inactive for extended periods.
- Temperature and Glucose Meter Accuracy: Extreme temperatures can affect the accuracy of glucose meters. Direct sunlight and high temperatures can alter the performance of the glucose meter and test strips, potentially leading to inaccurate readings. It’s important to keep your glucose meter and testing supplies within their recommended temperature range to ensure reliable results.
- Monitoring and Adjustments: When sunbathing, especially for extended periods, it’s crucial to monitor your blood sugar levels more frequently than usual. This allows you to catch any fluctuations early and make necessary adjustments to your diet, insulin dose, or activity level.
To manage blood sugar levels effectively while sunbathing:
- Stay Hydrated: Drink plenty of water to prevent dehydration, which can also affect blood sugar levels.
- Monitor Regularly: Check your blood sugar levels more often than usual, especially if you’re experiencing changes in activity or temperature.
- Protect Your Supplies: Keep your glucose meter and test strips away from direct sunlight and within the recommended temperature range specified by the manufacturer.
- Adjust Insulin and Diet: Be prepared to adjust your insulin dose or meal plan based on your blood sugar readings and activity level.
On the glaciers
- Insulin absorption can vary throughout the day, starting slowly initially and potentially increasing rapidly later on.
- Shivering to maintain warmth consumes more energy, which can lead to hypoglycaemia (low blood sugar levels). It’s advisable to wear layered clothing to regulate temperature, adjusting layers as needed to prevent overheating or excessive cold.
- Hypoglycaemia poses greater risks in cold conditions as it disrupts the body’s efforts to stay warm, increasing the likelihood of hypothermia.
- Cold temperatures can affect the accuracy of glucose meters, potentially yielding unreliable readings.
- For individuals with poor circulation or neuropathy, preventing frostbite is crucial. Insulin should not be used if it has been frozen and thawed, as this can impair its effectiveness. To prevent freezing, store insulin at room temperature or keep it close to your body, such as in an inside pocket, to ensure it remains unfrozen
Diabetes and Road Travel
- Before traveling, check your blood glucose levels and continue to monitor them regularly during your journey.
- If you experience initial signs of hypoglycaemia while driving, pull over immediately and only resume driving once your blood sugar has returned to a safe range.
- Limit your daily driving to a maximum of 12 hours or ensure you do not go longer than 6 hours between meals to maintain stable blood sugar levels.
- Maintain consistency in your medication schedule, meal times, and snack times as much as possible throughout your trip.
- Pack sufficient food in case there are delays in meal times to ensure you have access to appropriate nutrition when needed.
Diabetes management in travel
| Oral hypoglycemics No dose adjustment required for travel |
| Insulin: regular / long-acting insulin regimens No dose adjustment if < 5 time zone change Westward travel: longer day requires more insulin Eastward travel: shortens day, requires less insulin |
| Insulin: basal / immediate acting regimens Easier to manage changing time zones May be injected immediately prior to a meal |
Time zones and Medicines
- Some insulin pumps, CGMs, or Freestyle Libre devices may require manual adjustment of the time or date to ensure accurate delivery of basal insulin doses.

If travelling West

If travelling East

If on Pre-mixed insulin
Twice Daily Pre-Mixed Insulin Travel Instructions:
- Pre-Departure:
- Take your usual insulin dose at the normal time before departure.
- Obtain an insulin pen with rapid-acting insulin before your trip.
- During Travel:
- Check your blood sugar levels every 4-6 hours.
- If your blood sugar level is above 200 mg/dL, administer a correction dose, preferably with a meal.
- Upon Arrival in New Time Zone:
- Continue the above routine until you are in the new time zone.
- Administer the second injection of pre-mixed insulin at the same local time as you would at home (e.g., if you take it at 6 PM at home, take it at 6 PM in the new time zone).
- Alternative Option:
- Consider switching to a basal-bolus regimen prior to travel for better flexibility and control.
Diabetes complications and travel
Neuropathy:
- Risk of foot injury due to unaccustomed walking and inappropriate footwear (e.g., sandals, hiking boots, new shoes).
- Emphasize the importance of daily foot examinations and proper foot care.
- Advise against using new footwear for travel; ensure shoes are well broken in before the trip.
- Recommend alternating footwear.
- Encourage frequent changes of cotton socks in hot climates.
- Suggest standby antibiotic therapy in case of infection.
Retinopathy:
- Be aware of the potential for transient worsening of vision due to hypoxic retinal ischemia at high altitudes or during flights.
Nephropathy:
- Increased risk of renal failure if dehydration occurs.
- Adjust doses of prophylactic or standby medications accordingly
CME INDIA Learning Edge
| Instruct patients to carry adequate supplies in their original packaging. |
| Calculate travel duration and account for time zone changes. |
| Preferably switch to a basal-bolus regimen and split the basal dose, or continue with a premixed insulin regimen with correctional mealtime doses. |
| The goal is to prevent hypoglycaemia during transit. |
CME INDIA Tail-Piece
Read another CME INDIA hit story – Pearls to know about travel in diabetes:
Further Readings:
- Younis AS, Abouammoh NA, AlBreacan LM, Aldigi Y, Kadi A, Almohideb N, AlAmari N, Almigbal TH. Safe Travel Practices and Awareness among Diabetic Patients. J Environ Public Health. 2023 Jan 31;2023:6353086. doi: 10.1155/2023/6353086. PMID: 36761247; PMCID: PMC9904899.
- Mullin, Rachael, et al. “Navigating travel with diabetes.” Cleve Clin J Med 85.7 (2018): 537-542.
- Alduraibi, Rabia Khalid, et al. “Knowledge, attitudes, and practices of primary health care physicians regarding the pre-travel counselling of patients with type 2 diabetes in Riyadh, Saudi Arabia.” BMC Family Practice 21 (2020): 1-9.
- Centers for Disease Control (CDC).Managing diabetes in the heat Available from:https://www.cdc.gov/diabetes/library/features/manage-diabetes-heat.html.
- https://cmeindia.in/pearls-to-know-about-travel-and-diabetes/
- https://www.endocrinepractice.org/article/S1530-891X(20)35403-3/abstract
- Rajkumar, Venkatraman. (2023). Travel with Diabetes: A Comprehensive Review for Clinicians. Dubai Diabetes and Endocrinology Journal. 28. 10.1159/000527144.

Discover CME INDIA

- Explore CME INDIA Repository
- Examine CME INDIA Case Study
- Read History Today in Medicine
- Register for Future CMEs


Very nice comprehensive description for diabetics during travel
Hi